Which Covid Patients Get Monoclonals? CDC Study Spots Big Disparities.
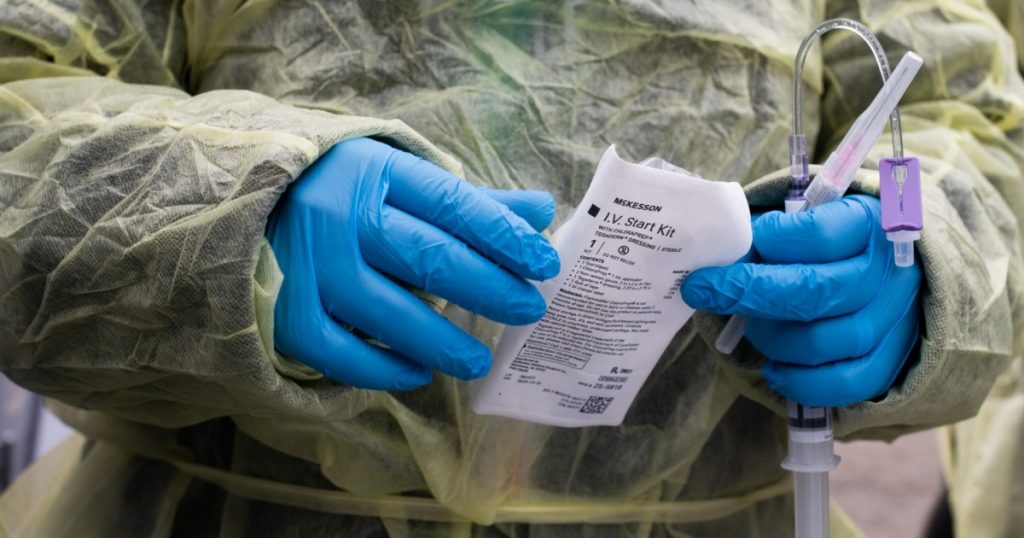
A healthcare worker prepares an infusion for a patient at a drive-thru monoclonal antibody treatment in the parking lot of Wayne Health Detroit Mack Health Center in Detroit, Michigan, Dec. 23, 2021.Bloomberg/Getty
Fight disinformation. Get a daily recap of the facts that matter. Sign up for the free Mother Jones newsletter.At this point in the pandemic, it’s clear the coronavirus has taken a disproportionate toll on people of color. Black, Latino, and Native Americans have been more likely than white Americans to be infected, hospitalized, and ultimately die of Covid-19.
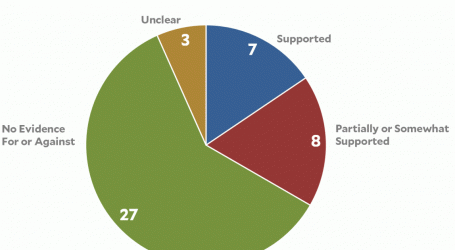
But until now, it was unclear whether rates of treatment with drugs known to be at least somewhat effective—monoclonal antibodies, dexamethasone (a steroid), and the antiviral drug remdesivir—followed the same disparity trends. In a recent report from the Centers for Disease Control and Prevention, scientists analyzed data covering more than 800,000 patients across 41 health care systems from March 2020 to August 2021. And the results are concerning, especially for the monoclonals, which have been shown to help prevent hospitalizations in high-risk patients.
Overall, only a small number of patients each month—4 percent or less, on average—received monoclonal antibodies. But there were clear disparities as to who got them: On average, Black and Asian patients were treated with monoclonals 22 percent and 48 percent less often, respectively, than white patients. Other races, including Native Americans and Pacific Islanders, were treated 47 percent less often than white patients. Hispanic patients were treated with monoclonals 58 percent less often than those who were non-Hispanic. In fact, during nearly every month the researchers measured, white patients were more likely than the other groups to be given the potentially life-saving treatment. This chart sums it up:
Percentage of Covid patients who received monoclonal antibody treatment by race and ethnicity.
CDCThe disparities for dexamethasone and remdesivir were “different and of lesser magnitude” the authors note, with Hispanic patients receiving dexamethasone 6 percent less often than non-Hispanic ones, and Black patients receiving remdesivir 9 percent more often than white patients.
The authors also cite limitations to the study, including that it was common for race and ethnicity data to be left off of records for people who tested positive, and that patient records were largely gathered from centers within the health care system, meaning they may not reflect trends among patients treated outside of those settings, such as government-run infusion sites.
The study suggests several possible reasons for the differences in monoclonal antibody treatment rates, including racial differences in access to transportation, testing, and care; “inadequate insurance coverage;” supply issues; “potential biases in prescribing practices;” and a lack of messaging in communities of color about the availability of the treatment.
Yet another possibility, as my colleague Edwin Rios aptly put it, is that, here in America, racism seems to be a preexisting condition.