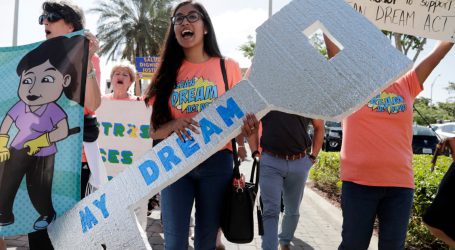Doctors Are Being Told That Wearing Masks “Might Freak Out Patients”
For indispensable reporting on the coronavirus crisis and more, subscribe to Mother Jones’ newsletters.As hospitals face a wave of patients with COVID-19, Dr. Christopher Garofalo, a family physician in Massachusetts, has become increasingly concerned about physicians working without masks and other protective equipment. In private Facebook groups for doctors, Garofalo asked them to share their experiences—and he received a torrent of responses from health care workers who said that hospital administrators forbade them from wearing the gear. The reasons for this vary: Some administrators say hospitals are afraid the gear could spread the virus to uninfected patients; others say administrators are worried that patients will be scared if they see doctors wearing masks.
Garofalo spoke to Mother Jones about the problem and provided some of the anonymous stories he has collected from health care workers. His remarks have been edited for length and clarity.
On his work: I’m a family physician in Massachusetts. I am a part owner of a private practice family medicine group called Family Medicine Associates of South Attleboro, which is on the Rhode Island border. I do general family medicine within that. And I also still deliver babies. That’s part of my old my practice of family medicine. It’s sort of a dying breed.
On what his office is doing right now: We have actually switched over to telemedicine. We are doing both phone visits with patients as well as video visits with patients, which helps to decrease the transmission, but it still provides them a way to have a face-to-face visit with somebody. The human interaction is really critically important in primary care.
We are a private office. I don’t work for a hospital. No hospital is going to fire me. That’s part of the reason why I can talk to you and a lot of other docs can’t.
On what he began to see in physician Facebook groups: I chair a group that’s called the Committee for Sustainability of Private Practice. Our goal is to keep private practice alive. I am also on several other private practice groups.
I started seeing some things on there about physicians who were saying, “I got yelled at by an administrator because I wore my mask in the hallway. And it’s going to scare patients. So I was told to take it off.” One of them had actually seen an email from the administrators that said, “We’re going to talk to the doctors to rein them in.”
I don’t know why it just hit me. Rein them in. Why would they want to do that? We try not to be arrogant, but physicians are some of the most educated people in the country. So I posted that in one of my groups. And I got responses that I had never seen before. And everybody started flooding with this story and that story.
On what hospital administrators are telling doctors: Here are a few of the stories that physicians sent to Garofalo on Facebook. Garofalo passed them along to Mother Jones without identifying information:
“We are being expected to walk into ERs with no N95 respirators provided to care for non-COVID emergencies (appendixes, hot gallbladder, etc) and when we complain or ask for a mask to be provided they’re telling us tough luck. One of our hospitals even sent an email saying do not divulge any positive cases, or else we could be found of violating HIPAA.”
“I was asked to remove the mask as it would frighten patients to think I was infected.”
“Hospital administrators have asked physicians and nurses not to take standard precautions to prevent spread of COVID—masks, staff temperature checks—that might freak out patients.”
“I asked specifically about what if i was concerned that i may be an asymptomatic carrier and was essentially told that i should not wear a mask for the protection of my colleagues and patients. on this conference call one hospitalist expressed concern that his wife has significant tracheal stenosis and he worried he might transmit the virus to her. he stated that he had been wearing an N95 mask w/highly suspected cases. he asked if he could reuse an N95 mask to protect his wife and was told flat out ‘no’ he could not, essentially because if they allow an exception in his case, they might have to allow others an exception as well.”
“[The hospital has] a supply of N95 masks that the nurse manager has locked up. Over the last shift, I had to see 5 COVID suspects-tests pending. I asked for one N95 to reuse as I know we have them. they refused as those are only for aerosol procedures—the only one they define as aerosol is intubation. Subsequently I got emails from admin to meet so they can tell me how to work with nursing directors and change my behavior. I have not responded yet. The ed physicians are not being given N95, even for intubation. One of them has reused his for 6 shifts. There was a code on a COVID patient and nurses and respiratory therapists were unprotected during active intubation, etc. Nurses are telling me that they have been forbidden to wear the blue paper masks for non-respiratory patients even though many are asymptomatic for up to 2 weeks. They are told they will be fired if they do. Pregnant social worker wore a blue mask and was told to take it off. I’m afraid for my job as well as the staff. They are expecting a surge and we don’t have enough blue paper masks and soon will run out of gowns. I have to be anonymous for fear of retaliation.”
“St. Anthony’s Hospital in Oklahoma City has asked us not to wear masks in the halls.” (Mother Jones called St. Anthony’s to ask about this policy, and the hospital responded, “At SSM Health St. Anthony Hospital, our priority always is to protect our staff and our patients. For this reason, we adhere to CDC best practice guidelines when determining the circumstances that require our staff to wear personal protective equipment, including masks. Established infection prevention protocols offer guidance to our providers regarding when it is appropriate to wear personal protective gear and when it may not be appropriate, such as for prolonged periods or in public places such as hallways, where such masks may become contaminated and potentially cause risk for both patients and the provider wearing their mask. We will continue to evaluate and update policies as this pandemic evolves.”)
On why these doctors are afraid to speak out: Nobody wanted to go on the record. They did not want me to put any information in there. They didn’t want to send a memo or even a screenshot, because even if you remove the names, depending upon what other information might be in there or what the format of the memo looks like, that could be discoverable and noticeable.
When they’re employed by the big hospital systems in Boston or Pennsylvania or California, their paychecks come from them. They can’t speak out without fear of losing their job.
If you lose your job, it’s not just that you could lose your livelihood. You could also be labeled disruptive, and that can lead you to disciplinary action, which can get reported to the board of medicine, and you could lose your license.
We know that most doctors are employed by large hospital chains. We know that administrators don’t value physicians. They value us only insomuch as they can get us to work for them. But they know they have us over a barrel. If you as a physician are told to see more patients and you speak up, all of a sudden, you become, quote, disruptive. You’re labeled disruptive. The balance has shifted, and physicians don’t have the autonomy they used to have.
On his hope that hospital administrators will change their policies on doctors wearing masks: The tide has turned a little bit. For example, Partners HealthCare in Boston basically said everybody is wearing at least a surgical mask, period. Everybody, no matter where you are—you’re just wearing one. In our office we’re going to do this next week.